Transparency in Coverage
Price Transparency: Unlocking Better Payment Rates
The Transparency in Coverage (TiC) rules were designed to force health plans to publish the secret payment rates they agree upon with doctors and hospitals. This data is the key to successful healthcare contract negotiations.
Why This Information is Hard to Use
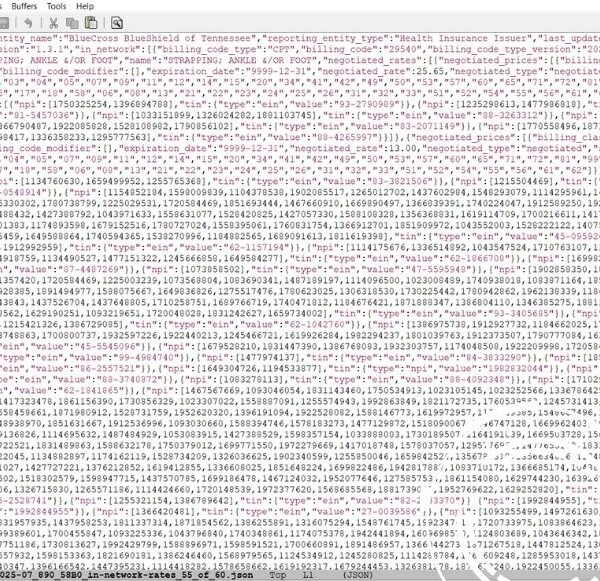
Even though this pricing data has been public since mid-2022, it's virtually unusable for a regular doctor's office trying to increase medical practice revenue:
-
Jumbled Files: The data is scattered across thousands of huge, complex, and poorly organized files.
-
Bad Data: The information is often incomplete or contains confusing "ghost rates" that aren't real.
-
No Standards: There's no easy way to plug this data into a system or compare it directly.
Because of these issues, most medical practices are still blind when they try to negotiate with insurance companies.
Reveon Health: The Clear Advantage
Reveon Health cuts through the chaos. We take this massive, flawed government data and turn it into simple, clear intelligence. This empowers providers to stop guessing, successfully negotiate with insurance companies for fair rates, and finally increase medical practice revenue.
Who this helps
Independent Practices
Small and independent practices gain local insights into market data of comparable practices and provider network options in their region, helping maintain autonomy.
RCM Teams
RCM teams have new tools to optimize the financial health of the practices they serve, supplementing billing and underpayment efficiency metrics with reimbursement rate intelligence.
Contract Negotiators
Contract negotiators have access to regional and local data to build the most effective negotiation posture on behalf of their clients.
Timeline of TiC


