How Reveon Health Simplifies Healthcare Cost Transparency

You can have two practices in the same zip code, same specialty, same CPT codes, same payer. And the reimbursement rates are still… all over the place. Sometimes by a little. Sometimes by a lot. And unless you have a very specific mix of data, experience, and time, you end up negotiating based on vibes.
That’s the whole reason cost transparency became such a big deal in the first place.
But here’s the part people do not say out loud enough. Having transparency data “available” is not the same as having it be usable.
Transparency in Coverage, or TiC, cracked open something important. It put negotiated rates into the daylight, at scale. The problem is, the daylight is coming through a firehose. And most provider orgs do not have a practical way to turn that into contract leverage.
That’s where Reveon Health shows up.
Reveon Health is building a healthcare data and benchmarking platform that takes TiC rate data, cleans it up, and turns it into reimbursement benchmark reports you can actually use in payer negotiations. Especially if you are a smaller practice without an army of analysts. Or if you are a consultant or RCM team that needs consistent benchmarking across clients.
This article breaks down what TiC is, why it matters, what usually goes wrong when people try to use it, and how Reveon Health simplifies healthcare cost transparency into something you can act on.
What “Transparency in Coverage” really means in the real world
TiC is a federal requirement that pushed health insurers to publish machine readable files that include negotiated rates.
Not chargemaster rates. Not the sticker price nobody pays. Actual contracted rates, by payer, by plan, by provider, tied to billing codes.
So, in theory, TiC answers questions providers have had forever:
- What does this payer pay other providers in my market?
- Are my rates in line with similar practices?
- Which codes are underpaid relative to local norms?
- Where do I have negotiation leverage?
In practice, TiC can answer those questions. But only if you can process it.
Because TiC files are massive, inconsistent, and messy. And that’s not an insult, it’s just the reality of how insurers publish data at scale. They are not publishing it in a “helpful for negotiations” format. They are publishing it to comply.
So the opportunity is huge, but the usability gap is even bigger.
The “cost transparency” gap nobody warns you about
Most people run into the same wall after the initial excitement.
They hear: “Negotiated rates are public now.”
Then they try to actually use the data, and it turns into:
- Downloading gigantic files that time out.
- Fighting file formats and naming conventions.
- Struggling to match payers, plans, and networks to what you actually contract under.
- Trying to compare apples to apples across codes and provider types.
- Getting stuck at “we have data” without a clean benchmark to reference.
And then, because the workflow is painful, the negotiation strategy stays basically the same as it was pre TiC. A few internal reports, maybe a consultant’s limited dataset, a payer meeting where everyone talks past each other.
So when we talk about cost transparency, the real question is not “Is it available?”
It’s “Can your team turn it into leverage fast enough to matter?”
Why TiC rate intelligence is suddenly a revenue lever
A lot of organizations still treat contracting like a periodic administrative chore. Renewals come up, you argue, you sign, you move on.
But reimbursement pressure has not been letting up. Labor is expensive. Denials are not getting easier. And payers have gotten very comfortable saying no.
If your contracted rates are even slightly off market, across a big enough volume, you feel it.
TiC rate intelligence changes the dynamic because it gives you external evidence, not just internal frustration.
Instead of “we need more,” you can move toward:
- “Here’s how our rate compares to comparable providers in this geography for this code set.”
- “These specific codes are materially under benchmark.”
- “This discrepancy is inconsistent with market norms and network parity.”
That’s not just transparency. That’s negotiation ammo.
Where Reveon Health fits in (and what it’s actually doing)
Reveon Health is positioning itself as a credible source for TiC rate analytics and benchmarking, for two main audiences:
- Independent and small practices that want the same intelligence without building an internal analytics stack.
- Large RCM teams, PMS platforms, and contract negotiation consultants who need repeatable benchmarks.
The core idea is simple, but it’s not easy to execute:
Take insurer TiC machine readable files and transform them into clear, local, specialty relevant reimbursement benchmarks.
And then package those benchmarks into reports that support real contract conversations.
The practical problem Reveon Health solves: turning TiC chaos into clean benchmarks
TiC files are raw ingredients. Reveon is the kitchen.
Instead of forcing a provider or consultant to deal with the messy steps, our platform is designed to give you something closer to:
- Your payer rates compared to local benchmarks
- Specialty specific views (so you are not comparing yourself to the wrong peers)
- Clarity on where you are underpaid, overpaid, or inconsistent
- Something you can export, share, and bring into negotiations
That is what “simplifying cost transparency” really means here. Not simplifying the concept. Simplifying the workflow and output.
A quick visual of the difference (raw TiC vs usable rate insight)
Here’s a simple way to picture it.
If your current process feels like “download files, parse, clean, pivot, double check, and still not trust it,” you are not alone.
Reveon’s value proposition is basically: stop doing that.
What “benchmarking” means, specifically, for reimbursement
Benchmarking in this context is not a generic national average that feels irrelevant.
Useful benchmarking tends to be:
- Local, because rates vary heavily by geography
- Specialty aware, because provider types matter
- Code specific, because negotiations are won and lost in CPT level details
- Grounded in real contracted rates, not billed charges
A benchmark report that can say “you are at the 25th percentile for these high volume codes vs similar providers in your market” is a different thing than a vague “your rates seem low.”
That difference matters in a payer meeting.
This need for clarity and specificity in healthcare pricing underscores the importance of Reveon Health’s innovative approach.
The hidden benefit: you stop negotiating blindly
A lot of practices negotiate based on a general sense that reimbursement is “not great.” Or they pick one or two codes and push on those because someone told them to.
But payers are not paying you one blended rate. They are paying you a thousand tiny rates that add up.
TiC derived benchmarks can surface patterns like:
- A payer that pays fine on E/M codes but is weak on procedures
- A network where your newer contracts are better but legacy plans are dragging you down
- Specific codes where you are far below what peers are getting, which can become your negotiation anchor
This is the stuff that changes outcomes. Because it’s specific and hard to wave away.
Why this matters for small independent practices (not just big health systems)
Big systems can sometimes brute force contracting with scale, brand leverage, and internal analytics.
Small practices are often stuck in a tighter box:
- Smaller contracting team (sometimes it’s just the administrator)
- Less time to do analysis
- Less patience for payer runarounds
- Less visibility into what “good” even looks like in their area
Reveon’s positioning here is important. It’s trying to make rate transparency usable for organizations that do not have a data warehouse and an actuary.
Because the truth is, small practices are often the most exposed to underpayment. A few points off on reimbursement can be the difference between “stable” and “constantly stressed.”
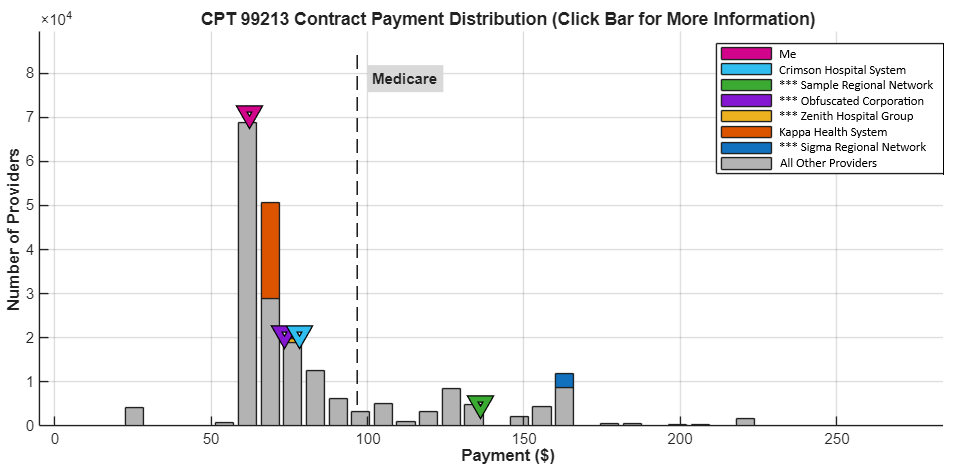
For RCM firms, consultants, PMS platforms: why credibility and consistency matter
If you negotiate for multiple practices, you know the pain.
You need benchmarks you can trust. You need consistency across clients. You need a way to explain your logic. And you need to produce something presentable, not a messy spreadsheet that only your analyst understands.
TiC is an appealing data source because it’s broad. But broad data is worthless if you can’t normalize it.
This is where Reveon is clearly aiming to be an authoritative and credible layer in the middle.
Not just “we have data,” but “we have cleaned and benchmarked rate intelligence you can use repeatedly.”
So what does Reveon Health actually output?
Reveon Health promotes reimbursement rate benchmark reports derived from TiC data.
The output is built to answer provider contracting questions like:
- How do my contracted rates compare to local norms?
- Where are the biggest gaps, by code and payer?
- Which payers show the largest underpayment patterns?
- What should I prioritize in negotiation?
And the key part. It’s meant to be clear.
Not just correct. Clear enough to take to a payer conversation, or to use internally when you’re aligning leadership around a negotiation strategy.
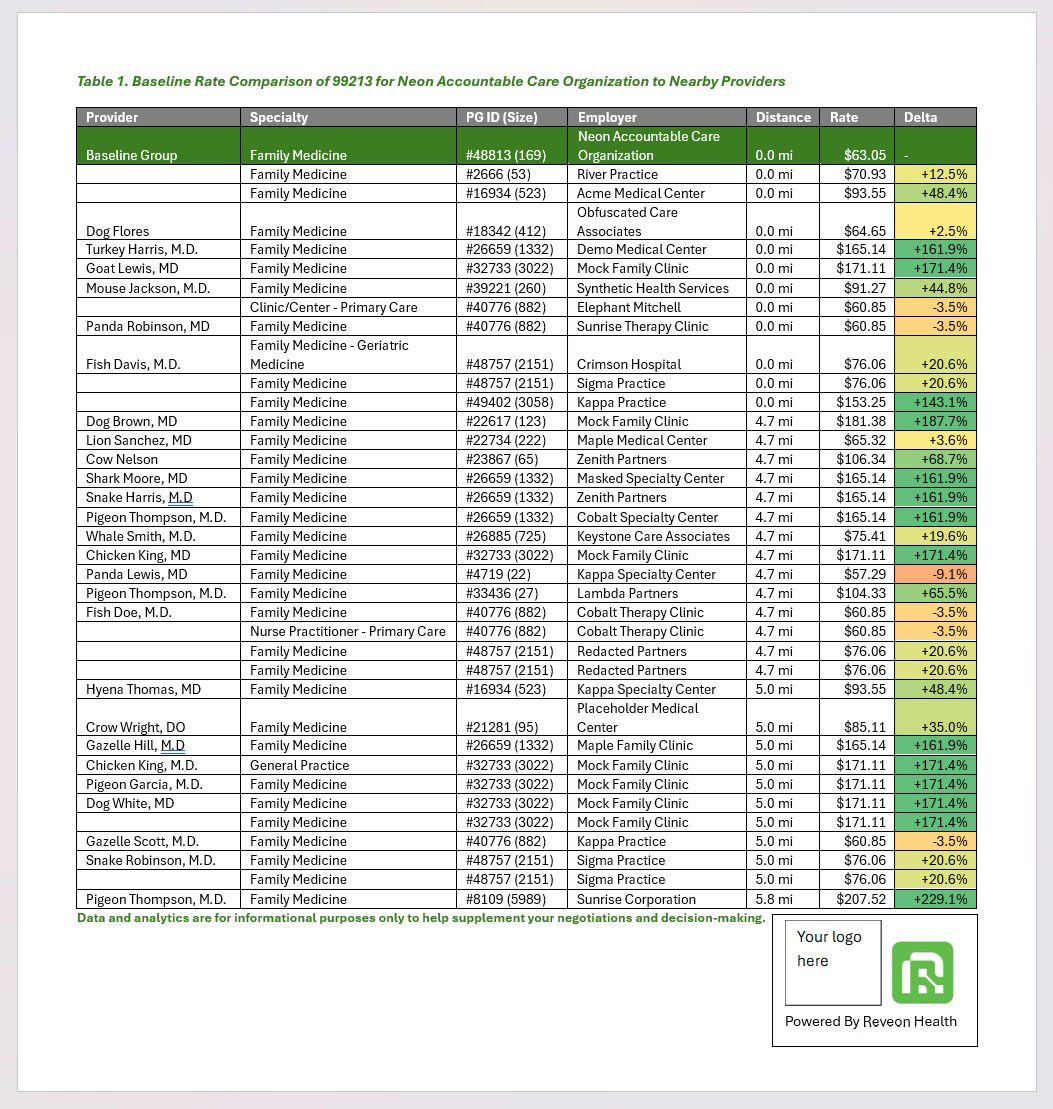
How “cost transparency” becomes a negotiation workflow
One of the biggest missed opportunities with transparency data is not embedding it into a workflow.
Teams pull data once. Make a chart. Feel informed. Then negotiations happen months later and the chart is stale, or it was never granular enough to begin with.
A cleaner approach looks more like this:
- Baseline your current contracted rates (by payer, plan, code, specialty, geography)
- Compare to benchmarks using TiC derived rate intelligence
- Identify the codes and contracts that matter most based on volume and gap size
- Build a negotiation narrative that is specific and defensible
- Track changes over time so you know if renegotiation actually worked
Reveon is trying to make these steps dramatically easier, because those are where most teams get stuck.
A note on “authoritative” TiC analytics, and why it’s not just marketing language
If you want to be taken seriously in contracting, you need data that stands up to scrutiny.
That means:
- Clear sourcing (it came from insurer TiC files)
- Transparent methodology (how the benchmarks are calculated)
- Reasonable comparisons (local, specialty aligned)
- Consistent definitions (payer names, plan groupings, code mappings)
Payers will poke holes. They always do. Not always because they are right, but because delay is a tactic.
The more rigorous your benchmarks, the less room there is for “we don’t agree with your numbers.”
This is why a platform approach matters. You are not just grabbing random examples. You are building a repeatable evidence base.
Where this gets really interesting: finding underpayment you didn’t know you had
Underpayment is not always obvious.
Sometimes it’s hidden in:
- A subset of plans under a single payer
- Older fee schedules that never got updated
- Certain “routine” codes that quietly drive most of your volume
- Contract language that created unintended carve outs
TiC driven benchmarking can surface these issues faster than traditional methods because it is external and comparative by nature.
And when you find one meaningful gap, it tends to lead to another.
That’s one reason TiC analytics has become a hot topic in RCM circles. It’s not just about transparency for patients. It’s a provider revenue intelligence opportunity.
However, the real challenge lies in identifying these underpayments. Regular auditing of payer payments is crucial to ensure accurate reimbursement, which can help uncover hidden underpayments.
What to look for in any TiC benchmarking tool (including Reveon)
If you are evaluating platforms in this space, a few practical questions help.
- Can it benchmark my exact market, not a national average?
- Can it filter by specialty and provider type?
- Can it break down by payer and plan, not just payer brand name?
- Does it give code level insight, not only summary stats?
- Can I export or share outputs in a way that supports negotiation?
- Does it feel like something my team will actually use monthly, not once?
Reveon’s message is that it’s built specifically for this use case: contracting and negotiation, not general analytics.
A simple, subtle next step if you want to explore Reveon
If you are curious and you want to see how your rates stack up, the lowest friction move is to sign up and see our free demo video. Or, you can request a sample report from your area.
Start here:
And if you’re an RCM firm or consultant, it’s worth approaching it as a repeatable benchmarking layer you can apply across your book of business, not just a one off report.
Let’s wrap it up
TiC made negotiated rates visible. That’s the big shift.
But visibility alone doesn’t change revenue. What changes revenue is turning that visibility into benchmarks, and turning benchmarks into negotiation leverage.
Reveon Health is trying to close that gap by taking TiC rate data and turning it into clear reimbursement benchmark reports that providers, consultants, and RCM teams can use to identify underpayment, compare against local and specialty specific norms, and walk into payer negotiations with evidence.
Not a gut feeling. Not a generic benchmark. Evidence.
If you are trying to make cost transparency actionable, and not just another compliance headline, Reveon is worth a look.
FAQs (Frequently Asked Questions)
What is Transparency in Coverage (TiC) and why does it matter for healthcare providers?
Transparency in Coverage (TiC) is a federal requirement that mandates health insurers to publish machine-readable files containing actual negotiated rates by payer, plan, provider, and billing codes. It matters because it provides healthcare providers with unprecedented access to real contracted rates rather than chargemaster or sticker prices, enabling them to understand market benchmarks, assess if they are paid fairly, and identify negotiation leverage.
Why is having access to TiC data not enough for effective payer negotiations?
Although TiC data makes negotiated rates publicly available, the files are massive, inconsistent, and often messy due to insurers publishing data primarily for compliance. Providers face challenges like downloading huge files that time out, dealing with varied file formats and naming conventions, matching payers and plans accurately, and comparing codes across provider types. Without tools to process this data into usable benchmarks, negotiation strategies remain ineffective.
How does Reveon Health help healthcare providers utilize TiC data?
Reveon Health offers a healthcare data and benchmarking platform that cleans up raw TiC rate data and transforms it into clear, local, specialty-relevant reimbursement benchmark reports. This enables providers—especially smaller practices without extensive analytics resources—and consultants or RCM teams to leverage accurate market intelligence for more effective payer negotiations.
What are the common challenges providers face when trying to use cost transparency data from TiC?
Providers often encounter issues such as downloading large files prone to timing out, navigating inconsistent file formats and naming conventions, difficulty matching payer plans to actual contracts, comparing different provider types and billing codes accurately, and lacking clean benchmarks for reference. These challenges create a usability gap that hinders turning transparency into actionable negotiation leverage.
How can TiC rate intelligence become a revenue lever for healthcare organizations?
TiC rate intelligence provides external evidence of how a provider’s reimbursement rates compare with local market norms. Instead of negotiating based on internal frustrations or assumptions, organizations can present concrete data showing specific codes underpaid relative to benchmarks or discrepancies inconsistent with market parity. This shifts contract discussions towards evidence-based negotiations that can improve reimbursement rates and revenue.
Who benefits most from using Reveon Health’s TiC benchmarking platform?
Reveon Health serves two main audiences: independent or small practices that lack the internal analytics resources but want access to reliable reimbursement intelligence; and large Revenue Cycle Management (RCM) teams, Practice Management System (PMS) platforms, and contract negotiation consultants who require consistent benchmarking across multiple clients. Both benefit from simplified access to actionable TiC-based benchmarks supporting real contract conversations.
