Introduction
Negotiated commercial reimbursement rates have historically been difficult for market participants to benchmark at scale. Federal price transparency initiatives were designed to improve access to pricing information and support consumers, purchasers, and researchers.1
In June 2019, Executive Order 13877 directed federal agencies to advance health care price and quality transparency.2 Subsequent rulemaking led to the Transparency in Coverage (TiC) requirements, under which most group health plans and issuers must publicly post machine‑readable files (MRFs) that include in-network negotiated rates and out-of-network allowed amount information. As of July 1, 2022, these TiC MRF disclosures became broadly required and are typically updated on a regular cadence.
Early experience with TiC data has shown that the files are extremely large and can be challenging to analyze, and that users must make methodological choices (e.g., how to summarize multiple rates per provider-service observation). Prior analyses have also documented the presence of ‘unlikely’ provider‑service rate combinations (‘ghost’ or ‘zombie’ rates) and differences in reporting structure across payers.3 4 Centers for Medicare & Medicaid Services (CMS) has proposed changes intended to improve TiC data usability, including reducing unlikely provider‑service combinations and adding utilization information.5
Case Study Overview
In our first case study, Reveon Health seeks to study the question, “How does provider group size influence negotiated rate outcomes with insurance companies for office/outpatient setting?” To perform this analysis, we looked at TiC-provided data sets for three large insurance companies, United Healthcare (UHC), Aetna, and Cigna, who provide health insurance services widely across all states; we picked out a national PPO plan for each insurance. These insurance companies and plan files were chosen because they have national applicability and consistency within each insurance. Payer-level differences have previously been noted with these data files, but the available data for professional out-patient procedures was generally complete.4 Within each plan, we looked at a typical in-office visit code for evaluation and management (E/M) associated with a routine, low-complexity visit in which the provider spends 20-29 minutes of total time managing a patient, the CPT code 99213. This billing code is commonly used by many providers of different specialties and is a good representative billing code for study purposes; it is also less likely to have ‘unlikely’ provider-service rate combinations, since it is commonly used across many specialties. We used January 2026 data sets for this analysis. The unfiltered, raw machine-readable files used for this analysis totaled more than 400 GB of data.
Next, we filtered the data for this large data set to only look at contracted in-network reimbursement rates tied to an office outpatient setting and with no billing modifiers. We then distributed the data by state based upon the practice location of NPIs within each group as reported in the NPPES registry (https://npiregistry.cms.hhs.gov/search), and each rate was normalized by the average Medicare reimbursement rate for that state to control for regional cost differences between different states. When multiple rates were associated with the same group, we averaged the rates. We recognize that prior analyses have identified unlikely provider-service combinations that are prevalent across TiC data sets; because of the subjectivity of this filtering methodology, we are not filtering them in this analysis and specifically chose a commonly used billing code that would have minimal prevalence of unlikely combinations.
We separately analyzed four different regions – the Northeast, South, Midwest, and West, as defined by the United States Census Bureau. This differentiation by region was to ascertain the effects, if any, of regional trends in provider group sizes. Finally, we obtained the provider group size associated with each rate in every data file. This group size was the total number of unique providers receiving the same contracted rates within this group. We used the combined filtered data set to analyze the impact of provider group size on contracted in-network rate outcomes for this typical E/M visit code in different regions of the country.
Provider Group and Population Metrics
| Definitions
Provider group: the contracting entity in the TiC file’s provider-group structure; size measured as number of NPIs listed in that provider group Group/rate samples: a rate associated with a provider group observed in the TiC data set Provider/rate samples: an association between a provider and rate that is inherited by a provider’s membership in a provider group that has that same rate Group-weighted results: when summarizing distributions, we weighted each sample by provider group size so results reflect the distribution faced by a randomly selected provider in this data |
Across the three national insurance plans, we found a total of more than 99,000 provider group/rate combinations, which we will refer to in this study as samples, associated with the desired billing code. Some of the identified provider groups had similarity or overlap between one another; this is expected, since we used three independent national insurance plans, and many contracting groups negotiate multiple insurance contracts on behalf of their provider membership. Since there were three different insurance plans in the data set, there are many providers who appear multiple times in the data sets – usually against independent insurance plans. In total, there were more than 8 million provider/rate samples represented in the data set, with a median group size of 6 and an average group size of 85. These statistics do not tell the entire story, however, since more than half of the samples are in Bin 1 with provider group sizes between 1-9.
Table 1 shows the total number of group/rate and provider/rate samples in the data for each of the binned provider group sizes, rounded to three significant digits. We observed that the number of providers who are part of large contracting groups is relatively high, but the number of samples of those large provider groups is relatively small, which could lead to some skewed results in the data when looking at Bins 6 and 7, particularly when we sub-divide the data by state or region, where the sample size will be even smaller. The seven bins shown in this table are used consistently throughout the rest of this article.
Table 1. Total Group/Rate and Provider/Rate Samples Per Provider Group Size Bin
| Bin 1 | Bin 2 | Bin 3 | Bin 4 | Bin 5 | Bin 6 | Bin 7 | Total | |
|---|---|---|---|---|---|---|---|---|
| Provider group size | 1-9 | 10-99 | 100-299 | 300-999 | 1,000-2,999 | 3,000-9,999 | 10,000+ | All |
| Total group/rate samples | 59,200 | 27,800 | 7,240 | 3,380 | 1,090 | 293 | 70 | 99,100 |
| Total provider/rate samples | 197,000 | 904,000 | 1.25M | 1.79M | 1.79M | 1.37M | 1.11M | 8.41M |
We performed most of our analysis considering the entire population of providers, rather than provider groups, and we weighted the group/rate samples by provider group size. This provider weighting is not “unique provider weighting,” since providers can appear multiple times in the dataset. However, this weighting is more representative of the perspective of viewers likely to read this article. Viewed from this perspective, if you were to order all providers in the nation in these datasets by the size of the group they are contracting with, the median group size of the provider population is 1,072.
We considered four regions of the United States – Northeast, South, Midwest, and West – as defined by the United States Census Bureau.6 These regions are shown in Figure 1.
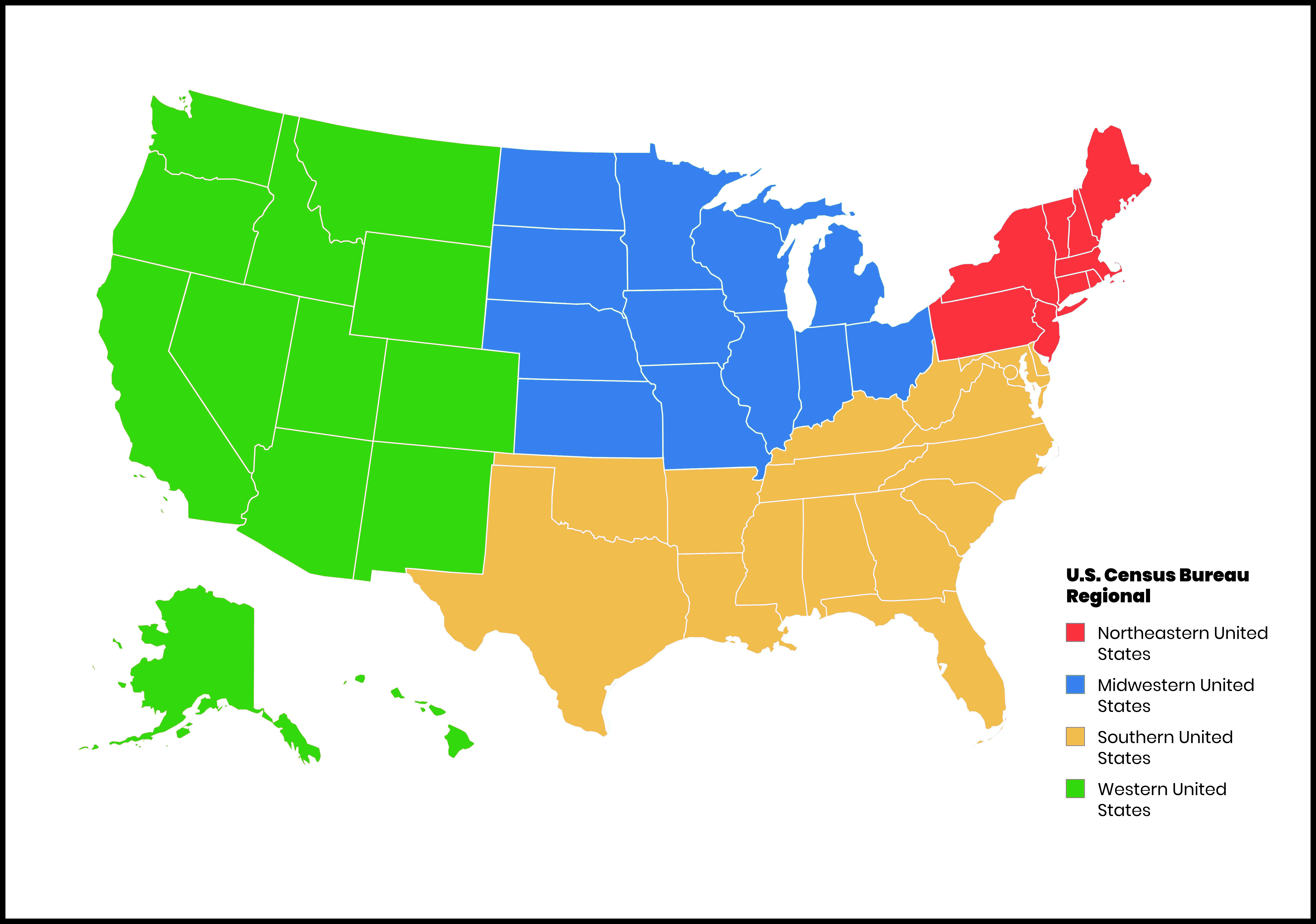
For each of the regions, we binned providers by their provider group size to calculate the distribution of provider group sizes across that region. We binned providers into the seven bins referenced above based upon the size of the provider group they are part of. For providers who appear multiple times in the data sets, we binned each occurrence separately; these situations represent appearance in multiple insurance plans or providers who have multiple associations, such as one who works in a small practice but has a separate affiliation for providing some services through a hospital. Figure 2 shows this distribution by region.
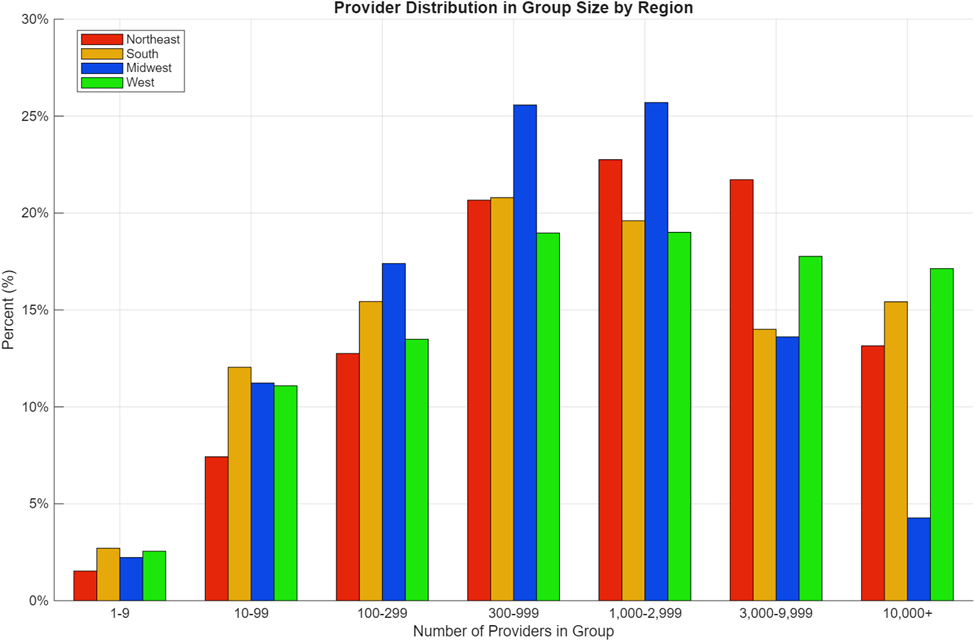
The distribution illustrates some regional differences in provider group sizes. When considering the entire population of providers, the 25th, 50th, and 75th percentile provider group sizes can give some additional insight; these are shown in Table 2. These metrics, like the prior graph, also consider the entire population of providers ranked by their group size. We can use the data below to show, for instance, that the middle half of the provider population in the Northeast is part of a contracting group between the sizes of 372 and 5,174 providers, with the median provider being part of a group of size 1,550. One could also use this data to conclude that 25 percent of all providers in the South are part of a contracting group smaller than 222 providers.
Table 2. 25th/50th/75th Percentile Group Sizes for All Regions
| Northeast | South | Midwest | West | |
|---|---|---|---|---|
| 25th Percentile | 372 | 222 | 227 | 255 |
| 50th Percentile | 1,550 | 952 | 765 | 1,284 |
| 75th Percentile | 5,174 | 3,812 | 2,200 | 4,655 |
Overall, this data illustrates a wide variety of provider groups. Analysis of the rate data against group size should be performed on a logarithmic scale and interpreted carefully for large group sizes, since the sample size of group/rate combinations is relatively small.
Overall Rate Distribution
Prior research using TiC data has documented substantial negotiated-price variation across geography, payers, and providers.7 8 For our analysis, we found 99,087 different rates associated with the desired billing code in the TiC data sets we analyzed from January 2026 – each rate associated with a provider group. The raw rate distribution showed an average non-group-size-weighted contracted in-network payment of $90 and a median payment of $79 across the US. These statistics answer the question, “What is the average/median contract group reimbursement rate?”. The group-weighted average and median reimbursement rates, answering the question, “What is the average/median provider payment?” were higher, at $106 and $84, respectively, reflecting the influence of larger negotiating groups. For this particular code, the average Medicare reimbursement rate across the US is approximately $88, but it can vary from $81 to $112, depending on state and locality.
The raw rate data itself can be biased by cost-of-living differences in the different regions being evaluated, so we normalized the rates by the average Medicare rate in that state. This normalization allows us to compare cross-state rate information to analyze correlations and trends. The average provider-group-size weighted contracted rate was 110% of the state’s average Medicare rate, and the median was 89%. However, the variation in payment rates was substantial, with a standard deviation of 58%! The distribution is not Gaussian, however, and exhibits a strong right tail. The distribution of these rates is shown in Figure 3 below.
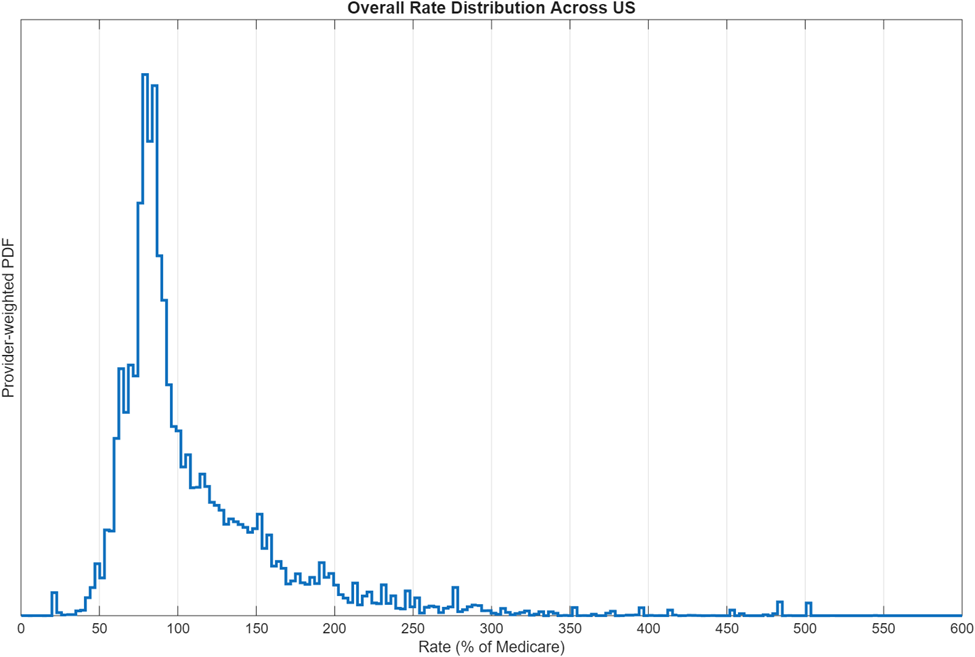
The distribution suggests that, while most providers are paid about a statistical distribution around Medicare reimbursement rates, there is a significant number of providers paid well above Medicare rates. About 7% of all providers receive payment rates above 200% Medicare rate for this code, and some providers achieve up to 500% of Medicare rate! Considering how profoundly in-network reimbursement rates can impact the financial wellbeing of healthcare businesses, it is critical for independent practices to understand correlation between controllable inputs (such as their negotiated insurance contracts or the decision to join a local clinically integrated network) and the desired output state (e.g., rates). We will analyze what effects provider group size has on rate, and whether there are regional influences or variations between insurances.
Insurance Analysis
We used data from United Healthcare (UHC), Aetna, and Cigna, three large national insurance companies to perform this analysis. While payer-level differences are not the focus of this study, we do briefly analyze differences in the distribution of reimbursement rates for CPT code 99213 between these insurers to assess the validity of aggregating data from all three insurers for provider group and rate association. We leave it to a future effort to perform more detailed analysis of rate outcomes by insurer. This section is not intended to rank insurers; it illustrates that negotiated-rate outcomes vary across payers in the TiC data.
First, we plot the entirety of the data set of each insurance, independent of state or region, against provider group size. This was done by aggregating the group/rate data normalized to Medicare percent for each insurance company, over every state, and computing a smoothed distribution against log-scale provider group size. Each insurance company is plotted as a ribbon; the coloring represents the inner two quartiles (25th-75th percentiles), and the solid line is the median. Figure 4 shows the results for all three insurance companies. All are plotted as a function of group size on a log scale. There are relatively low sample counts for the 7th bin (10,000+ providers), so variation is high in this range.
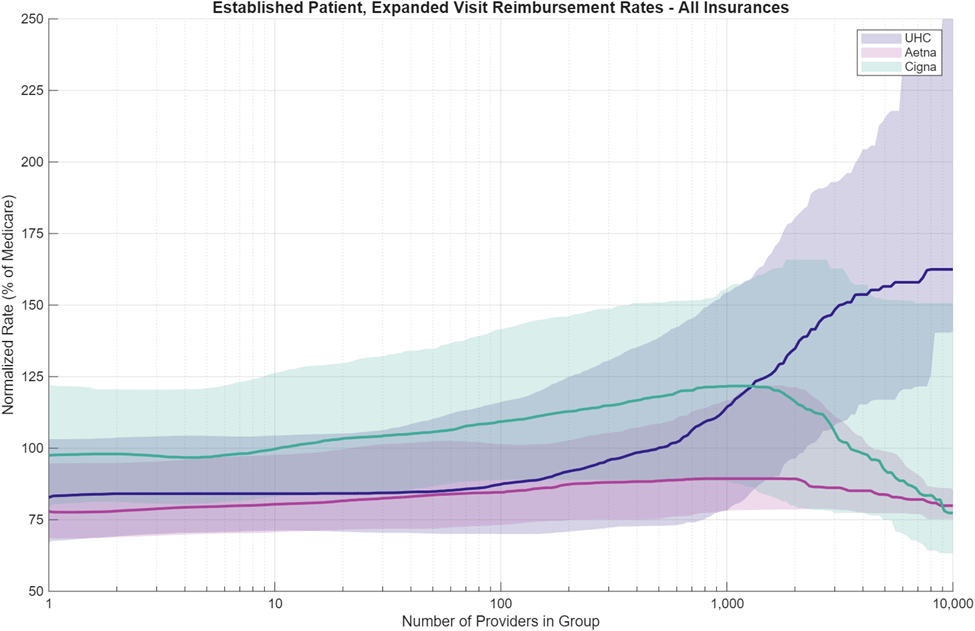
The graph above shows a positive correlation between group size and rate outcome for all three insurance companies from group sizes of 1 to 1,000 (Bins 1 through 4 in our analysis), but it is not consistent above 1,000 provider group size (Bins 5 through 7). For two of the insurance companies, rate outcomes reduce above 1,000 group size, but for one of the insurances, it continues to increase. This suggests that contract negotiation is not consistent between all insurance companies, and it is important for independent practices to have access to all TiC data to make informed decisions when negotiating their contracts and deciding whether to join a clinically integrated network. One possible explanation is differences in network composition or contracting structures across payers (primary care providers vs. mid-level providers vs. therapists, etc.) between the insurances. We recommend exploring this relationship further in a future study.
A few insurance-specific statistics are shown in Table 3, including the approximate sample size of each group size bin and the group-size weighted mean and standard deviation of each insurance, representing the distribution of rates expected for the population of providers in each bin.
Table 3. Statistics Comparing Rate Distributions for Three Different Insurance Companies
| Bin # | Group Size | United Healthcare | Aetna | Cigna | |||
|---|---|---|---|---|---|---|---|
| Mean ± Std. Dev. | Samples | Mean ± Std. Dev. | Samples | Mean ± Std. Dev. | Samples | ||
| 1 | 1-9 | 92±37% | 20,300 | 90±37% | 34,100 | 107±42% | 4,890 |
| 2 | 10-99 | 95±39% | 11,000 | 93±38% | 12,500 | 117±49% | 4,200 |
| 3 | 100-299 | 102±44% | 2,470 | 94±35% | 3,160 | 125±54% | 1,600 |
| 4 | 300-999 | 114±54% | 1,150 | 99±41% | 1,450 | 129±58% | 784 |
| 5 | 1,000-2,999 | 141±62% | 312 | 109±47% | 512 | 134±67% | 265 |
| 6 | 3,000-9,999 | 173±82% | 61 | 95±38% | 152 | 118±80% | 80 |
| 7 | 10,000+ | 317±135% | 3 | 82±24% | 58 | 165±126% | 9 |
| All | All | 125±69% | 35,400 | 95±39% | 51,900 | 129±71% | 11,800 |
Briefly comparing the insurance rate distributions, the average rates between the insurance companies differ by more than 30% overall. United Healthcare shows the strongest correlation between group size and rate. The average rate increases by a factor of 1.9x between Bin #1 (1-9 providers) and Bin #6 (3,000-9,999 providers). Aetna has a correlation between rate and group size, but it is a weaker relationship, with only a factor of 1.2x between Bin #1 and Bin #5 (1,000-2,999 providers). The relationship then decreases above 3,000 providers. Cigna shows a similar trend, with a factor increase of 1.25x between Bin #1 and Bin #5, and then a decrease in rate vs. group size above 3,000 providers. Note that, despite these trends, significant variation exists regardless of provider group size, so negotiated rate outcome depends on many variables – not just provider group size. The overall standard deviation of the rate distribution was between 39% and 71% for the three insurances, confirming that substantial amounts of the variation are not described by group size.
For the regional group-dependency analysis, data from the three insurance companies will be aggregated and considered in total.
Regional and Provider Group Size Dependence
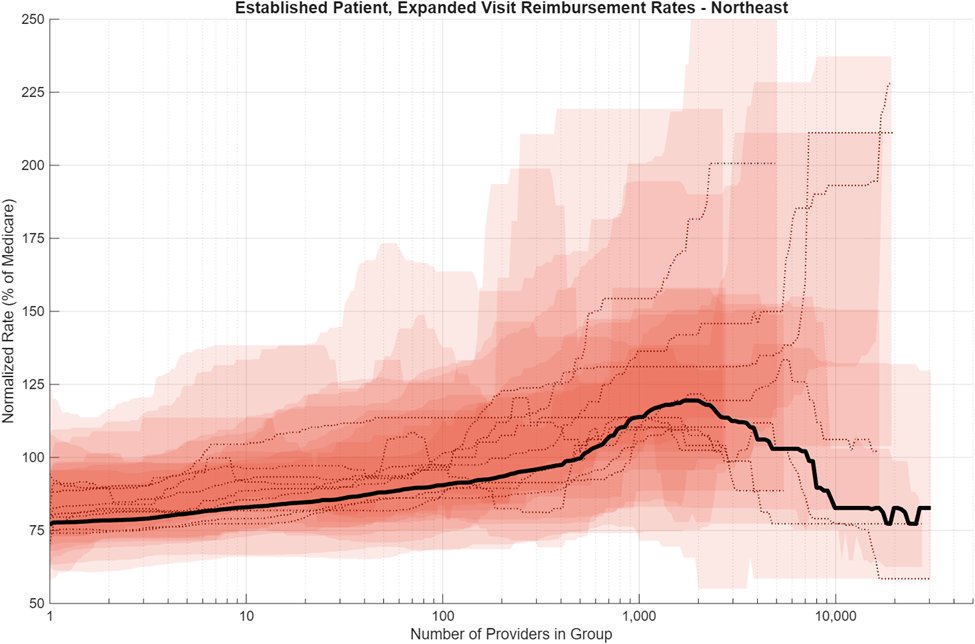
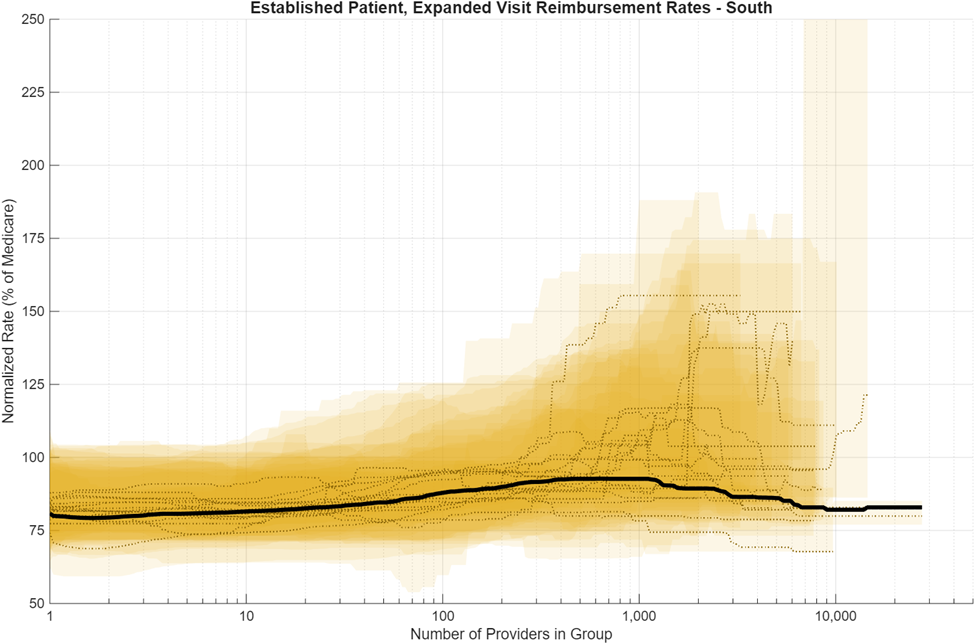
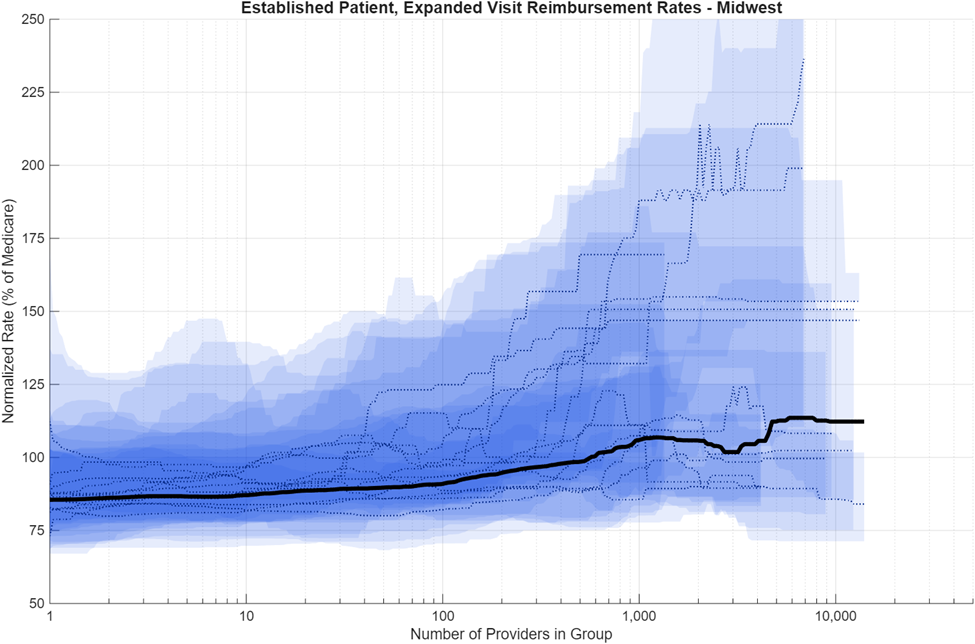
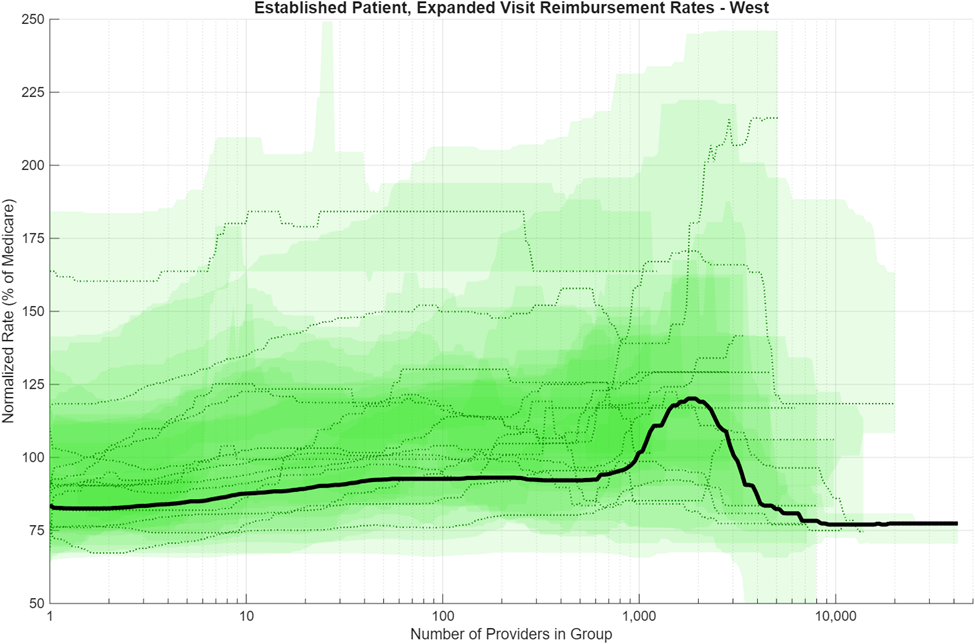
The data analysis is visualized in a series of plots below. Each figure shows a different region. Each ribbon represents the 25th to 75th percentile range of reimbursement rate outcomes for a different state in that region, and each colored line is the median reimbursement rate of that particular state as a function of provider group size. State-level data was combined for the three different insurance company plans to provide a large statistical data set for analysis. Some state-level variations exist; these are commonly caused by having a small sample size of large provider groups that in some cases heavily weight the relationship being analyzed. The solid black line in each figure shows the regional provider-weighted median for reference. All rates shown are normalized to the average Medicare rate for their state (in percent). Medicare Physician Fee Schedule (PFS) amounts vary by payment locality using geographic practice cost indices (GPCIs) applied to the work, practice expense, and malpractice Relative Value Unit (RVU) components. Even after normalization to state-mean Medicare rates, private negotiated rates show meaningful variation across states and regions. This regional variation is consistent with observations from prior studies that have been conducted.7
As with the ribbon plots in the insurance analysis, the regional ribbon plots also have small sample sizes in Bin #7, so be cognizant of the uncertainty and variation associated with distributions in this bin. Figures 5-8 illustrate the regional distributions by provider group size for the Northeast, South, Midwest, and West regions. Click the graphs to expand.
Figure 9 shows the overlay of the median regional distributions from each of the four prior graphs.
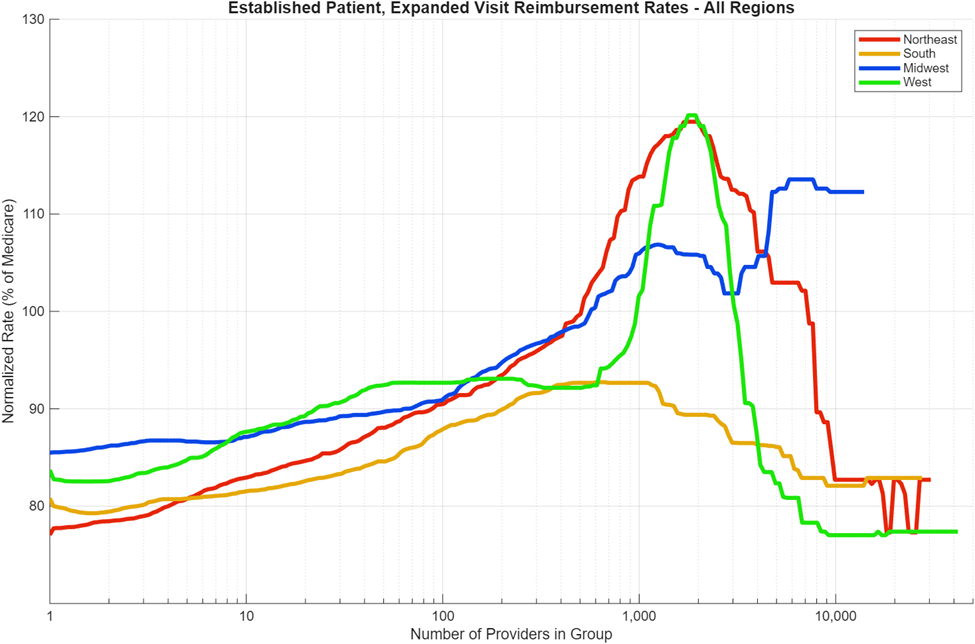
This regional data shows significant variation among the TiC data. Even within a region, it is not uncommon for state-to-state median payment differences of dozens of percent, which is surprising since Medicare locality code is intended to compensate for local variations in cost-of-living. We recommend deeper inter- and intra-regional comparison and analysis for a future study.
Correlation with Provider Group Size
In all regions, there is a clear positive correlation between provider group size and negotiated rate outcome for the E/M billing code being analyzed – up to a point. Some of the largest provider groups do not appear to offer much of an overall positive benefit to negotiated rate. As previously discussed in the insurance analysis, two of the three insurance companies showed a negative correlation for rate against group size above 3,000 providers. Positive correlation between group size and negotiated in-network rate is most noticeable between Bin #1 (1-9 providers) and Bin #5 (1,000-2,999), where median rates improve roughly linearly vs. log(group size), up to 33% higher. In these TiC data, median negotiated rates tend to increase with provider group size through the ~1,000–2,999 provider bin, but distributions overlap substantially—indicating group size is not determinative. Local, state, and regional distributions vary – and, as previously analyzed, trends among insurance companies also vary – so it is worth digging into the data within your region to ensure a CIN is available with better rates, and that the terms of the CIN agree with the personal preferences of the practice. Table 4 shows the improvement of median rates of all of the binned provider group sizes compared to Bin #1, the smallest provider groups.
Table 4. Improvement in Median Payment Rate for CPT 99213 Compared to Median Payment for Bin 1 (Group Size 1-9 Providers)
| Bin # | Group Size | Northeast | South | Midwest | West | National |
|---|---|---|---|---|---|---|
| 1 | 1-9 | - | - | - | - | - |
| 2 | 10-99 | +8% | +4% | +4% | +8% | +5% |
| 3 | 100-299 | +15% | +11% | +8% | +10% | +11% |
| 4 | 300-999 | +25% | +15% | +14% | +10% | +15% |
| 5 | 1,000-2,999 | +51% | +11% | +25% | +47% | +33% |
| 6 | 3,000-9,999 | +27% | +6% | +18% | -4% | +5% |
| 7 | 10,000+ | -4% | +3% | +70% | -9% | -3% |
Being part of a larger provider group alone does not guarantee positive rate outcomes. In fact, the correlation between provider group size and rate outcome, nationally, is only +0.06, and even excluding groups above size 3000, the correlation is still only +0.12! Thus, provider group size is only weakly beneficial to rate outcomes, and other variables at play not subject to this study likely have additional impacts on rate. Thus, additional exploration of the variability of rates against provider group size is necessary. A box-and-whiskers plot is useful to visualize this variability within the different provider group size bins, as shown in Figure 10.
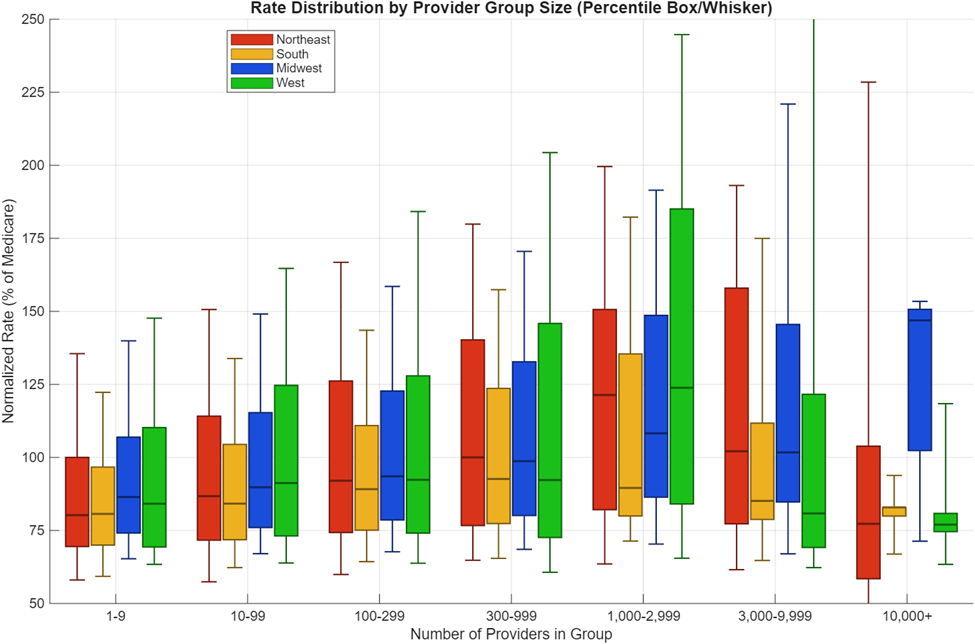
In this plot, one can see that there is substantial overlap between rate outcomes for each of the different provider group size bins, suggesting ample room for maneuvering for smaller independent practices to achieve positive outcomes. However, the negotiation advantages of being in a larger provider group are also readily apparent, as these groups have the possibility to achieve much higher objectives.
One way to quantify the rate advantage of larger groups is to consider a scenario in which a provider wishes to receive 200% of Medicare reimbursement rate. Nationally, this situation occurs for approximately 7% of all providers for the analyzed billing code. Diving into the TiC data shows that the situation is much more common for larger provider group sizes than smaller ones. Nationally, a provider is more than 4 times more likely to receive at least 200% of Medicare reimbursement rates in a provider group size of 1,000-2,999 in membership than he or she is independently as part of a small practice of 1-9 providers; in the West, where more than a fifth of providers in the provider group bin between 1,000-2,999 receive more than 200% of Medicare for this code, the improvement factor is more than 7x. Table 5 shows the likelihood of a provider reaching this threshold payment based upon the binned provider group sizes.
Table 5. Percent of Providers by Provider Group Size Who Make At Least 200% of Average State Medicare Reimbursement Rate for CPT 99213
| Bin # | Group Size | Northeast | South | Midwest | West | National |
|---|---|---|---|---|---|---|
| 1 | 1-9 | 2.5% | 1.8% | 2.6% | 3.0% | 2.3% |
| 2 | 10-99 | 3.0% | 2.1% | 3.3% | 4.5% | 2.9% |
| 3 | 100-299 | 6.1% | 1.9% | 3.4% | 8.1% | 4.1% |
| 4 | 300-999 | 7.1% | 4.2% | 4.5% | 11.2% | 6.1% |
| 5 | 1,000-2,999 | 9.6% | 6.0% | 7.3% | 21.8% | 9.9% |
| 6 | 3,000-9,999 | 8.8% | 4.2% | 12.6% | 16.8% | 9.5% |
| 7 | 10,000+ | 23.3% | 2.7% | 0.0% | 4.4% | 7.2% |
| All | All | 9.7% | 3.6% | 5.7% | 11.7% | 6.9% |
Conclusion
The case study analyzed by Reveon Health gives insight into the relationship between provider group size, insurance, region, and in-network outpatient reimbursement rates for a commonly used E/M billing code. This study was made possible through use of Transparency-in-Coverage (TiC) data that has historically only been accessible to hospitals and insurance companies due to proprietary restrictions but is now publicly available to all providers.
In our dataset, the median negotiated rate for groups in the 1,000–2,999 bin is approximately 33% higher than the 1–9 bin, with meaningful overlap in distributions. These results are descriptive and do not establish causal effects of consolidation or affiliation with larger groups. Group size is likely not the only variable that influences rate outcome, however, and further studies are needed to evaluate other effects that could account for more of the observed variation.
Further Studies
Further studies using similar data could dig further into relationships for other variables on rate outcomes, including:
- Other non-E/M billing codes and specialty-specific codes
- Taxonomy differences in provider groups and rate outcomes (e.g., primary care physicians, specialties, mid-level providers, etc.)
- State- and local-level differences in rates (e.g., urban vs. rural, hospital within 50 miles, etc.)
- Rate metrics and variability over time
- Consolidation trends in healthcare markets, both regionally and nationally, their association with rate outcomes for providers, and whether these trends improve patient satisfaction
- Insurance company and plan variations
Data quality enhancements for future work include:
- Implement a utilization-based screen to reduce unlikely provider-service combinations using publicly available utilization data or claims-based validation
- Estimate a regression or mixed model of normalized rates as a function of log(group size), payer fixed effects, and geography fixed effects to quantify partial associations
About Reveon Health
Reveon Health is a healthcare technology company focused on empowering providers with the data intelligence needed to maintain autonomy and financial sustainability. Built for independent practices, Reveon leverages intelligently analyzed Transparency in Coverage (TiC) data to help practices benchmark rates, evaluate networks, and negotiate smarter. This brief is part of an ongoing effort to make TiC data more usable for provider decision-making.
Additional information and self-service tools are available on our website at https://www.reveonhealth.com. If you have questions about this case study, we encourage you to contact us at support@reveonhealth.com or via our LinkedIn page (https://www.linkedin.com/company/reveon-health).
References
- (2025, August 14). Use of Pricing Information Published under the Transparency in Coverage Final Rule. Centers for Medicare & Medicaid Services. https://www.cms.gov/priorities/healthplan-price-transparency/overview/use-pricing-information-published-under-transparency-coverage-final-rule
- (2019, June 24). Executive Order 13877—Improving Price and Quality Transparency in American Healthcare To Put Patients First. U.S Government Publishing Office. https://www.govinfo.gov/content/pkg/DCPD-201900419/pdf/DCPD-201900419.pdf
- Claxton, G., Cotter, L., & Rakshit, S. (2025, February 25). Challenges with effective price transparency analyses. Health System Tracker. https://www.healthsystemtracker.org/brief/challenges-with-effective-price-transparency-analyses/
- Muhlestein, D. B., Pathak Y. (2025, December 12). Price Transparency With Gaps: Assessing the Completeness of Payer Transparency in Coverage Data. The American Journal of Managed Care. https://www.ajmc.com/view/price-transparency-with-gaps-assessing-the-completeness-of-payer-transparency-in-coverage-data
- (2025, December 19). Transparency in Coverage Proposed Rule (CMS 9882-P). Centers for Medicare & Medicaid Services. https://www.cms.gov/newsroom/fact-sheets/transparency-coverage-proposed-rule-cms-9882-p
- (2026, February 26). Census Regions and Divisions of the United States. United States Census Bureau. https://www2.census.gov/programs-surveys/economic-census/2022/geographies/reference-maps/2022-ec-regions.pdf
- Whaley, C., Radhakrishnan, N., Richards, M., Simon, K., & Chartock, B. (2025, January 21). Understanding health care price variation: evidence from Transparency-in-Coverage data. Health Affairs Scholar. https://academic.oup.com/healthaffairsscholar/article/3/2/qxaf011/7965202
- Chartock, B., Simon, K., & Whaley, C. (2023, October 27). Transparency in Coverage Data and Variation in Prices for Common Health Care Services. JAMA Network. https://jamanetwork.com/journals/jama-health-forum/fullarticle/2811063